April 13, 2022
Rethinking the Medicaid Managed Care Entitlement: A Home- and Community-Based Approach Expands Options and Improves Outcomes
Guest blog by Brendan Harris, Vice President of UPMC Community HealthChoices
UPMC is one of three Medicaid Managed Care Organizations (MCOs) participating in Pennsylvania’s statewide Community HealthChoices (CHC) program. Many of our UPMC CHC members have been diagnosed with chronic illnesses, frequently with multiple comorbidities, and are low-income, making them “dually eligible” for coverage through both Medicare and Medicaid. Eighty-six percent of our dually eligible members are from traditionally underserved communities (both rural and urban) and communities of color. Less than 10 percent of dually eligible beneficiaries are enrolled in plans that “align” their Medicare and Medicaid coverage. The remaining duals have separate Medicare and Medicaid coverage, that varies by state. The health care needs of this population are complex, and MCOs must think differently about how to best serve these individuals. Fortunately, there is a solution and the successes we have seen with our dually eligible members provides a clear road map to state and nation policymakers: With more alignment between managed care coverage under Medicare and Medicaid, you can truly and effectively serve this very vulnerable and underserved population.
Unlike traditional Medicaid, UPMC CHC coordinates non-traditional benefits, including long-term care and home- and community-based services (HCBS) for individuals with chronic, complex health conditions. HCBS can include personal care, adult day care, home-delivered meals and transportation services. Ensuring access to these services not only promotes a healthier, more independent life; it also reduces costly, avoidable hospitalizations and health care emergencies by focusing heavily upon preventative care and chronic condition management. HCBS also makes it easier for vulnerable individuals to “age in place” at home instead of having institutional care as their only option for long-term care. For members who wish to remain at home, HCBS can enhance quality of life and support greater independence. This refreshingly common-sense approach is becoming an increasingly important part of how we provide health care to low-income individuals living with chronic conditions.
UPMC CHC also is unique, in that we have more than 32,000 participants enrolled who also are enrolled in one of our Medicare products. As our UPMC Community HealthChoices Success Stories demonstrates, our integrated, clinically driven model of care makes UPMC CHC, and other similarly situated MCOs, uniquely qualified to offer a creative, “whole-person care” approach to best meet the needs of our members. This process starts with a comprehensive health assessment of each member that is reviewed by an interdisciplinary care team. This team develops a customized care plan that leverages our strong community-based relationships to enable access to all services necessary for independent living. UPMC CHC prioritizes long-term success by providing continued check-ins and communication to ensure each member’s needs are fully met and to proactively identify and address any emerging obstacles to care and independence. The infographic below illustrates how our teams harness numerous services and supports that may not be part of the traditional Medicaid program but that have major effects on our members’ health and wellness, independence and quality of life.
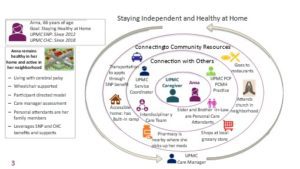
State and national policymakers are recognizing the value of this integrated approach. Pennsylvania’s CHC program has been operational since 2018, and more than half of all states now offer Medicaid coverage that includes access to long-term services and supports, like HCBS. This approach to coordinating care and HCBS is changing the conversation about how to best provide health care and support for underserved, vulnerable populations. With whole person care that aligns Medicare and Medicaid, you can de-fragment health care, but then when you include HCBS, it changes the fundamental nature of the Medicaid program, shifting it from a disjointed and institutional-based care driven model to one that also provides resources to give individuals the option to remain safe and healthy at home and in their community.
Ongoing discussions related to the “Build Back Better” reconciliation package include significant investments in HCBS—investments on top of the dollars committed to HCBS in the COVID relief packages passed during the height of the pandemic. These investments have and will continue to improve access, care and affordability, and otherwise help close health-equity gaps for many individuals located in underserved, rural areas, communities of color, seniors and the chronically ill. Programs like Pennsylvania’s CHC work to better and more cost-effectively support these vulnerable populations.

Brendan Harris is Vice President of UPMC Community HealthChoices (UPMC CHC), the state’s Managed Long-Term Services and Supports program for UPMC Insurance Services. Prior to joining UPMC, Harris served as a core member of the Department of Human Services (DHS) team for over a decade—a department that serves more than 3 million Pennsylvanians, operates with a $39 billion budget, and has over 16,000 employees.


































